Two newly introduced malaria vaccines have delivered striking results in Ghana, bringing the country closer to its long-standing goal of ending child deaths from the disease, according to the international vaccine alliance Gavi and Ghana’s health authorities.
However, sharp reductions in foreign aid—led by the Trump administration’s withdrawal from Gavi funding and scaled-back support from other wealthy donors—now risk limiting the vaccines’ reach across Africa, where malaria remains the leading killer of young children.
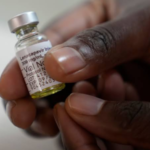
Malaria claims nearly half a million lives annually among children under five across the continent. Ghana, an early adopter, began piloting GSK’s RTS,S (Mosquirix) vaccine in select districts in 2019 as part of a WHO-led programme.
The second vaccine, R21/Matrix-M (developed by Oxford University and the Serum Institute of India), received WHO recommendation in 2023, accelerating wider deployment with Gavi support.
Measurable Impact in Ghana
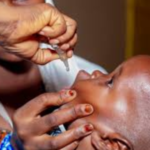
Dr Selorm Kutsoati, head of Ghana’s immunisation programme, called the malaria vaccine a “gamechanger.” Official figures show confirmed deaths among children under five plummeted nearly 86%—from 245 in 2018 (the year before RTS,S rollout in pilot areas) to just 35 in 2024.
A decade earlier, annual under-five malaria deaths averaged around 1,000. Malaria infections also declined significantly, falling from roughly 6.7 million cases in 2018 to 5.3 million in 2024, with about one-fifth among children under five.
While under-diagnosis and unreported home deaths mean actual numbers are likely higher, WHO’s malaria team lead for Africa, Dorothy Achu, confirmed the combination of vaccines, insecticide-treated bed nets, preventive drugs, and prompt treatment has driven a “significant reduction in malaria deaths.” Ghana’s data is now informing updated WHO global estimates.
Real-world evidence reinforces the impact: A January 2026 study published in The Lancet found severe malaria cases were 58% lower among vaccinated children in the year after receiving the third dose across pilot countries. Ghana achieved over 70% coverage for three doses in early 2025, among the highest rates reported.
Funding Crisis Threatens Wider Rollout
Gavi, the sole procurer of malaria vaccines for African countries, now faces severe constraints. Internal estimates prepared for its December 2025 board meeting (seen by Reuters) project Gavi will spend just over $800 million on malaria vaccines over the next five years—28% less than assessed need. The shortfall stems from a broader $2.9 billion gap in Gavi’s overall 2026–2030 funding goal.
The United States, previously Gavi’s largest donor ($1.3 billion from 2020–2024), withdrew support in June 2025 under Health Secretary Robert F. Kennedy, Jr., as part of foreign aid cuts aligned with President Trump’s “America First” agenda.
The U.S. has conditioned future funding on Gavi phasing out vaccines containing thimerosal (a mercury-based preservative), citing discredited claims linking it to autism—despite multiple studies showing no safety concerns. Gavi remains in contact with the U.S. government but insists portfolio decisions will follow “scientific consensus.”
Other donors have scaled back: the UK, Gavi’s biggest contributor, pledged £1.25 billion ($1.72 billion) for 2026–2030—over 20% less than its previous cycle. Gavi’s malaria programme head, Scott Gordon, said: “It is the gap between the promise and the need for the vaccine, and the resources we have to provide that.”
Gavi’s modelling (with Imperial College London and the Swiss Tropical and Public Health Institute) estimates an additional 19,000 child deaths over five years due to lower vaccination rates. Coverage varies: Ghana and Burkina Faso exceeded 70% for three doses in early 2025, while conflict-hit South Sudan reached only 35%.
Price Reductions & Domestic Efforts
Vaccine price cuts offer some mitigation: GSK and Bharat Biotech plan to reduce RTS,S costs to under $5 per dose by 2028 (roughly half current levels). Gavi and UNICEF secured a 25% reduction for Serum Institute’s R21 vaccine within a year. Burkina Faso, Ivory Coast, and Togo have committed to covering some needs domestically, but Tanzania has delayed its rollout due to funding gaps.
Dr Samwel Lazaro, acting head of Tanzania’s malaria programme, said the government is prioritising bed nets and other essentials while seeking solutions for vaccine financing.
Outlook & Challenges
Ghana’s success shows the vaccines’ potential when paired with existing tools. However, aid reductions threaten momentum in high-burden countries. Logistical challenges—multi-dose schedules, rural cold-chain limitations, and initial community resistance (overcome in Ghana through testimonies)—require ongoing support. With funding tightening, the challenge is ensuring progress against one of Africa’s deadliest killers is not reversed.


























































































































































































































![MMIA Fire: Keyamo Inspects Lagos Airport After Terminal 1 Blaze Disrupts Flights Hon. Festus Keyamo SAN arrives MMIA past 11:50 p.m. Feb 23 to lead oversight of Terminal 1 fire. Joined FAAN MD & team actively managing situation. Directed morning inspection Tuesday to guide restoration & confirm safety standards. Reaffirmed focus on passenger safety. Story: [link] #KeyamoMMIA #FireIncident #FAAN](https://fullcliphq.com/wp-content/uploads/2026/02/mym-150x150.jpg)